

Dear Colleagues,
Doncaster LMC has reviewed the recent communication regarding proposed changes to the diabetes specialist nursing service, including the expectation that general practice may assume responsibility for insulin adjustment in people with diabetes. The letter explicitly references a “process in primary care… when patients need insulin adjustments” and a “step down from DSN team to primary care once ready for discharge.” These statements indicate a shift of insulin titration into routine general practice.
Following discussion at the full LMC meeting, we want to be clear that this work does not sit within the core GP contract, and any shift of insulin titration or modification into primary care represents a significant transfer of workload, clinical risk, and liability to practices. Insulin management requires specialist expertise, carries significant clinical risk, and is not resourced within existing contractual arrangements.
At this stage:
Practices should continue to provide care in line with the existing GP contract and refer patients requiring insulin modification to specialist services as usual.
We will update you as soon as further information is available.
NHS England has confirmed the final GP contract arrangements for 2026/27. The package focuses on GP capacity, same‑day access for clinically urgent needs, QOF reform, vaccination changes, and new data and engagement requirements.
For further information please follow this link on the Doncaster LMC website https://www.doncasterlmc.co.uk/gp-contract-summary-2026-27

Directs access Fibroscan referral forms for Montagu Hospital have now been added to e-systems for all Doncaster practices. These updates will go live across all EMIS sites within the next week, with SystmOne already updated.
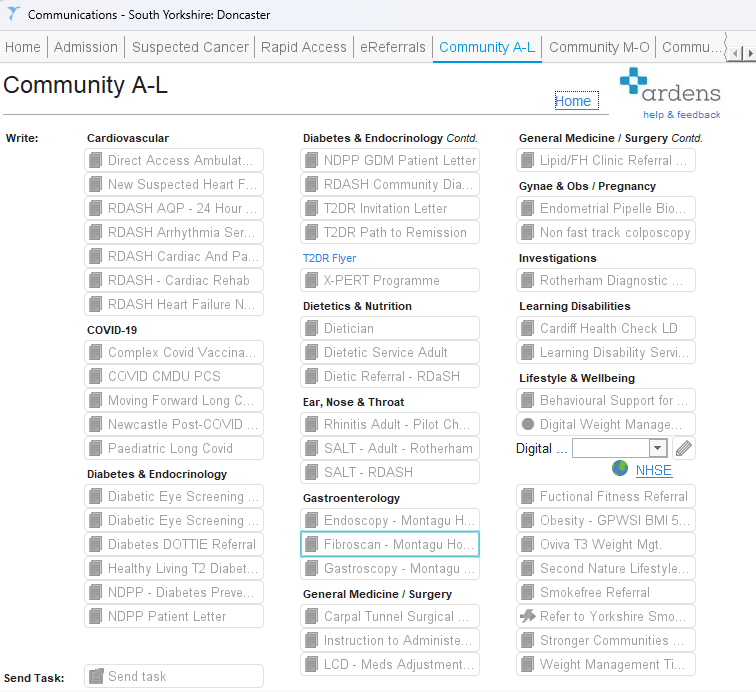
Practices can now access the referral forms in the following locations:
Guidance is available for anyone who needs a reminder on how to access referral documents using the F12 key.
Click here to view the step‑by‑step instructions.
These updates ensure that all Doncaster practices are using the most current referral pathway for Fibroscan services delivered at Montagu Hospital. This supports:
The following information has been supplied by Kirsten Brown from VWV.
Is the legal title to the property in the full legal names of current partners?
GP Partnerships cannot register their legal title to a property at the Land Registry in the name of the Partnership. They must therefore name between 2 – 4 individual partners who hold the legal title to the Property on trust for the Partnership.
It is important that this is kept up to date with any partnership changes as keeping retired partners on your property documents can present difficulties in dealing with the property in the future (e.g. if you were to grant a lease or sell the property and were no longer in contact with a former partner).
Is your Partnership Agreement up to date?
Your Partnership Agreement should be kept up to date with details of your properties and any agreements reached between the partners on how the properties will be held and managed.
Have you informed your Bank of any departures or new joiners in the Partnership?
Most GP Surgery premises will be subject to a legal mortgage. The Bank will need to be kept informed of any changes in the Partnership to ensure their loan and mortgage documentation is up to date and in the names of current partners.
Is your buildings insurance correct?
Your buildings insurance should:
Do you have a ‘Display Energy Performance’ (DEC) certificate and is it on display in the surgery premises and is the rating at least level ‘E’?
A DEC is required for any building that is larger than 250 square meters and is occupied by a public authority, this includes GP surgeries.
The DEC must be displayed openly for the public to see at the property.
Do you have an asbestos report to show that you have identified and are managing any asbestos risks at the Property?
Many GP Surgeries were developed at a time when asbestos was still commonly used. Unless the premises is fairly modern, there should be an asbestos report in place and the Partnership should be managing the risks identified in accordance with the report’s findings and recommendations.
Do you have the required risk assessments in place?
A GP Surgery should have the following risk assessments in place which are kept under regular review and should manage any risks identified accordingly:
If you are a tenant of your premises, have your rent reviews been carried out and properly documented?
Many GPs lease their surgery premises. GP Surgery leases usually provide for rent reviews to be undertaken every 3 years. It is important to ensure that rent reviews are undertaken in a timely fashion and are properly documented to avoid outstanding reviews (and subsequent outstanding rent payments) accumulating.
Are any third parties who regularly use space in the property properly documented (a licence or lease arrangement)?
It is common for GPs to share use of their premises with other healthcare providers without any formal documentation being in place. It is important that such agreements are documented to ensure that any third parties who use your premises do not gain any unintended rights over the premises.
Are the rent reviews up to date in any Leases to third party occupiers?
It is common for GPs to grant leases to third parties, such as dentists or pharmacies. It is important to ensure that these leases are properly managed and, in particular, that the rent reviews due under these leases are undertaken as they fall due and are properly documented.
Are you recovering all the financial contributions you are entitled to from occupational tenants? For example, insurance/service charges/rates?
Many GPs Surgeries are shared with third parties, such as other healthcare providers, pharmacies and dentists, who may have an obligation under their leases to contribute towards the cost of items such as insurance, utilities, rates and services. You should ensure that you are collecting the contributions which you are entitled to.
Have any occupational leases or licence arrangements expired? Or are any about to expire?
If you lease a GP Surgery, or have granted a lease or licence to a third party (e.g. a pharmacy), it is important to keep an eye on the expiry date of that lease or licence to ensure that it is renewed before it’s expiry.
If you would like more information please contact Kirsten Brown in the Healthcare Commercial Property team. VWV solicitors.
The national flu vaccination programme letter for 2026 – 2027 has now been published, setting out the eligibility criteria, programme timings, and vaccine recommendations for the upcoming autumn/winter season. The guidance is aimed at all organisations responsible for commissioning and delivering the NHS seasonal flu programme in England.
Winter remains the period of highest pressure on health and care services, with respiratory viruses peaking and placing significant strain on urgent care, primary care, and community services. The national letter emphasises that increasing vaccination uptake across all eligible cohorts is essential to protect the most vulnerable and maintain system resilience.
There are no changes to the eligible cohorts for this season. Eligibility continues to follow Joint Committee on Vaccination and Immunisation (JCVI) advice.
Employers are expected to ensure easy access to vaccination for all eligible frontline staff and to monitor uptake.
JCVI has reviewed the latest evidence and confirmed that all preferred vaccines for this season are trivalent. Key updates include:
Commissioners will actively recover payments where incorrect vaccines are used for a cohort.
NHS England has now confirmed its intention to transfer all remaining direct commissioning functions to Integrated Care Boards (ICBs) from April 2027, subject to the required legislative changes. This marks the next major step in establishing ICBs as the strategic commissioners for almost all NHS services, with only the most highly specialised areas remaining nationally commissioned.
The letter provides a clear roadmap for the transition and describes the leadership role expected of ICBs throughout 2026/27, ahead of the formal transfer. It also introduces the creation of seven Offices for Pan‑ICB Commissioning (OPICs) – regional hubs designed to support commissioning at scale, strengthen expertise, and ensure consistency across systems.
These OPICs will be hosted by one ICB in each region and will bring together the specialist commissioning workforce currently based in NHS England’s regional teams. They are expected to be fully operational by April 2027.
Subject to parliamentary approval, the following services will move from NHS England to ICBs:
This represents a significant expansion of ICB responsibility, building on the earlier delegation of primary care commissioning in 2022 and 2023.
Once NHS England is abolished (expected in 2027), the Department of Health and Social Care (DHSC) will take on responsibility for:
DHSC will also maintain national service specifications, standards, and clinical commissioning policies to ensure consistency.
ICBs are expected to:
This transition year is intended to ensure a smooth handover and avoid disruption to service delivery.
Please be reminded that practices are required to submit data for the six Quality Improvement (QI) indicators (highlighted below) in the Quality and Outcomes Framework (QOF) 2025/26 service.
This data is required to be submitted in order for CQRS to calculate an achievement for the QOF 2025/26 service. If practices do not provide the required information for these QI indicators by end of day (EOD) on 1st April 2026, QOF 25/26 achievement will not calculate at year-end due to missing data and calculation will be delayed until entered.
Please follow the steps below to submit manual data for the QI indicators in CQRS:
N.B As these QI indicators are noted as being retired from the Quality and Outcomes Framework 25/26, submitted responses will not be subject to review, however a response is still required for a successful achievement calculation.
Please note that if you are one of the small number of organisations that require manual entry for all indicators, please ensure this is done by EOD 1st April 2026.
Please see QI indicator descriptions for your information below:
QI Indicators | |
Indicator | Description |
QI013 | The contractor can demonstrate continuous quality improvement activity focused upon workforce and wellbeing as specified in the QOF guidance |
QI014 | The contractor has participated in network activity to regularly share and discuss learning from quality improvement activity focused on workforce and wellbeing as specified in current QOF guidance. This would entail attending two primary care network meetings, at the start and towards the end of QI activity. If a practice is not within a PCN, the expectation is that two meetings would be held locally with other practices |
QI016 | The contractor can demonstrate that it has in place a recognised and validated approach to understanding demand/activity, capacity and appointment data and has made improvements to data quality to better reflect practice work. |
QI017 | The contractor can demonstrate that it has utilised demand and capacity data to inform operational decisions and plan for demand and capacity matching |
QI018 | The contractor has participated in network activity to review the smart cards of all staff employed under the Additional Roles Reimbursement Scheme (ARRS), to ensure that the staff role assigned on their smart card aligns with the role they are employed under within the ARRS. |
QI019 | The contractor can demonstrate improvement in reducing avoidable appointments by |
Powered By EmbedPress
Tirzepatide (Mounjaro®) Kwikpen in adults 18 years and over with type 2 diabetes mellitus, amber G guidance document V2.0 has been updated and approved at the IMOC meeting . The update included an update to the pancreatitis, orlistat and retinopathy sections and addition of the flow chart from PCDS as an appendix.
Powered By EmbedPress
The SY Gluten Free Prescribing position statement is now live on the medicines Optimisation website.
SYICB does not recommend the routine prescribing of gluten free food products for use in coeliac disease, confirmed gluten-sensitive enteropathies and dermatitis herpetiformis or other gluten intolerances in South Yorkshire. SY IMOC Traffic Light Status: GREY (gluten free products should not be prescribed in South Yorkshire unless exceptional circumstances apply).
Powered By EmbedPress
From March 2025, new Simpler Recycling requirements will apply across England. These changes affect general practice premises and other primary care sites as “relevant non-domestic premises”. Please follow this link to the Doncaster LMC website for further information regarding what practices need to know, what is changing, and the practical steps to take. https://www.doncasterlmc.co.uk/simpler-recycling-in-england
Are you a new or aspiring partner (GP or non-GP) in South Yorkshire looking to thrive in your role?
The GP Partner Launchpad is designed to unlock your potential, empower you to lead change, and equip you with the essential business and leadership skills needed for a successful career in partnership.
What the scheme covers:
Delivered by:
Education leads from the SY Workforce & Training Hub, SY LMC Executives, and other experts.
Join the 2026/27 Cohort:
Please express your interest by the end of May.
Register your interest here: https://yhtraininghubs.co.uk/south-yorkshire/south-yorkshire-schemes/gp-partner-launchpad/
Under 18s
Refer to RDaSH CAMHS services
Referral Process Information: Child and adolescent eating disorders – Rotherham Doncaster and South Humber NHS Foundation Trust (RDaSH)
Over 18s
SYEDA
Accept presentations of Binge Eating Disorder and mild / moderate presentations of Anorexia Nervosa (BMI over 17.5) and Bulimia Nervosa (frequency of purging less than x 5 a week) where there are no significant broader MH concerns. Young persons with ARFID who are under the age of 25 with a BMI of over 17.5.
Referral Process Information: SYEDA – South Yorkshire Eating Disorder Association
Doncaster CMHT
Where there are significant broader mental health concerns (reaching the threshold of CMHT support) alongside eating disorder presentation; specialist clinicians are available within the Doncaster CMHT provision.
Referral Process Information: Adult community mental health – Rotherham Doncaster and South Humber NHS Foundation Trust (RDaSH)
Specialist Eating Disorders Service (SEDS)
SEDS – Accept moderate / severe presentations of Anorexia Nervosa (BMI under 17.5 / rapid weight loss) and Bulimia Nervosa (frequency of purging more than x 5 a week) and patients where there are additional risk factors (e.g. pregnancy / poorly managed diabetes) and patients who are transferring from another specialist eating disorder service.
Copies of required blood tests need to be sent with the referral form for triaging (currently SEDS can not access ICE results for Doncaster patients).
Referral Process Information: Eating Disorder Service | Sheffield Partnership University NHS Foundation Trust
Currently there are very limited commissioned services for ARFID in the SY region. ARFID presentations that meet SYEDA acceptance criteria and are under the age of 25 can be assessed for suitability for a pathway offered by SYEDA – South Yorkshire Eating Disorder Association
Doncaster LMC is been a member of the LMC Buying Groups Federation.
Buying Group membership entitles practices to discounts on products and services provided by the Buying Group’s suppliers.
Membership is free and there is no obligation on practices to use all the suppliers. However, practices can save thousands of pounds a year just by switching to Buying Group suppliers. To view the pricing and discounts on offer you need to register for access to the Buying Group’s online portal: https://buying.plexusportal.co.uk/Register.
What is the purpose of the Buying Group and how does it work?
The sole purpose of the Buying Group is to save its member practices money by negotiating discounts on goods and services which practices regularly purchase. The Buying Group team negotiate with suppliers, after which they identify ‘approved’ suppliers, who guarantee to give you significant discounts over what you would otherwise pay for their services, in return for the Buying Group’s endorsement and help in making you aware of what they offer.
Does it cost us anything to be part of the group?
No, membership is free and members are free to use as many discounts as they wish.
Is there any obligation to take up the deals offered?
No. Each practice is free to take up or decline any of the deals the Buying Group have negotiated. If you wish to take advantage of any of the offers in question, you will be given contact details, and all communications take place between you and the individual supplier*.
*The Buying Group accepts no liability for any contract willingly entered into by a practice with an approved supplier. Practices are advised to check that the terms of any contract with suppliers are consistent with those the Buying Group have negotiated and are advised to inform the Buying Group team of any discrepancy. The Buying Group do not, however, accept any responsibility for any member practices’ failure to check the terms of the relevant contract and the principle of caveat emptor (buyer beware) applies in all cases. Your rights as a consumer under the Consumer Protection Act are unaffected. With respect to any services to which the provisions of the Financial Services Act 2000 might apply practices are advised to seek independent financial advice as may be appropriate.
What happens to my details?
When a practice signs up for Buying Group membership, they will keep your basic contact details (practice address) on a secure system. On the membership application form, they also ask you how they can use your personal data (i.e. your email address) but even if you do sign up to receive their emails you can stop them at any time by clicking the unsubscribe button.
What if I am not happy with the quality of goods and services supplied?
Always let the Buying Group know if you encounter any problems getting what you want, and they will endeavour to sort it out.
Contact the Buying Group
The Buying Group is managed by Plexus Support Services Ltd:
Tel: 0115 979 6910
Email: info@plexussupport.co.uk
Website: https://www.plexussupport.co.uk
Welcome to Doncaster LMC. We use cookies to enhance your experience, analyse site traffic, and personalise content. By clicking 'Accept,' you consent to our use of cookies. You can manage your cookie preferences or withdraw consent at any time by adjusting your settings. For more details, please review our Cookie Policy Learn more